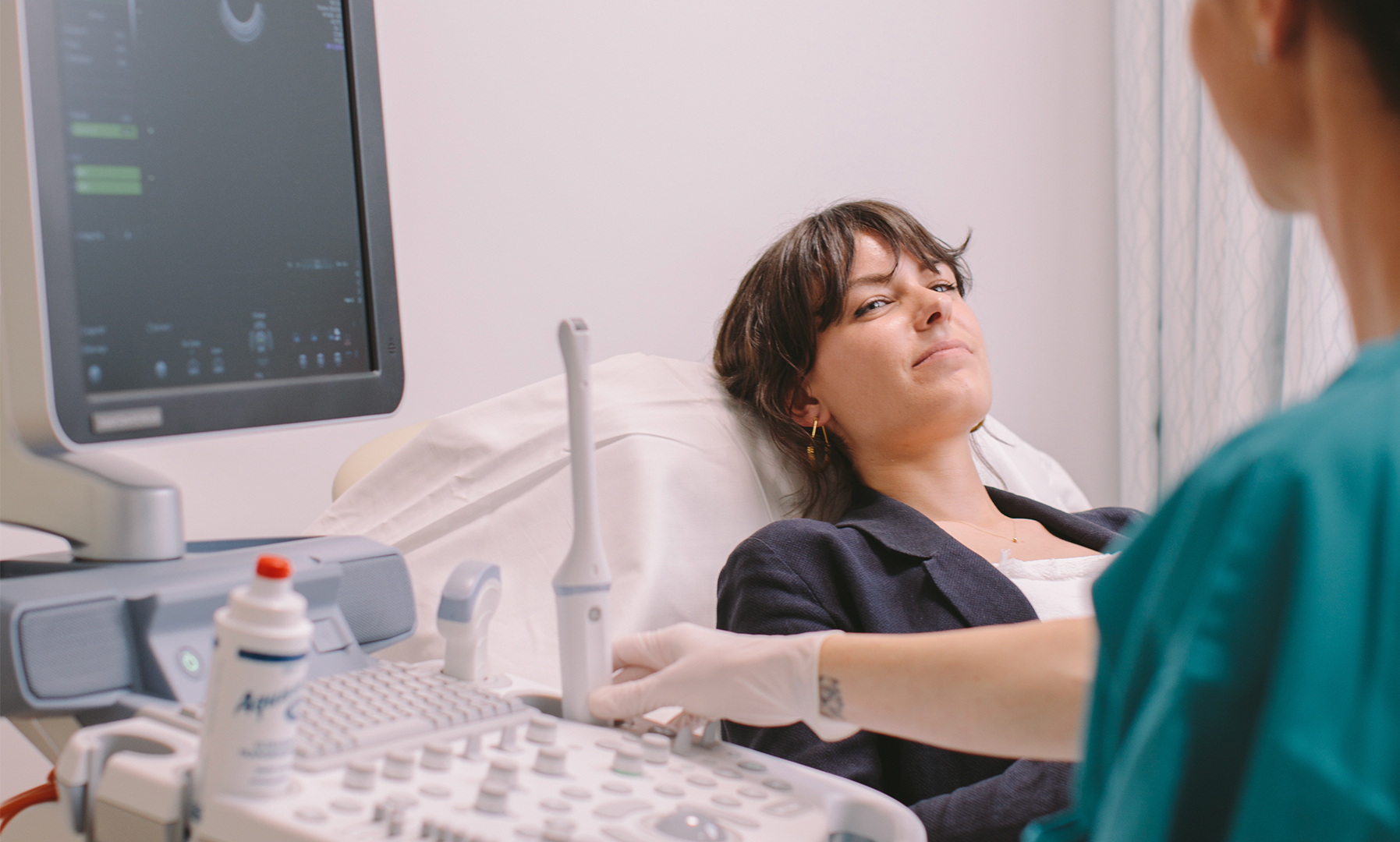
Services
We offer comprehensive fertility services with a single goal in mind: to help you achieve your dream of having a baby. But we won’t push fertility treatment on you if you don’t need it. We believe in maximising your chances of a successful pregnancy using the very least amount of intervention possible.

Services we offer

Start your fertility journey
Wherever you are on your journey, one of our supportive nurse enquiry team can help you understand your options and take the next step. These conversations are free and informative.